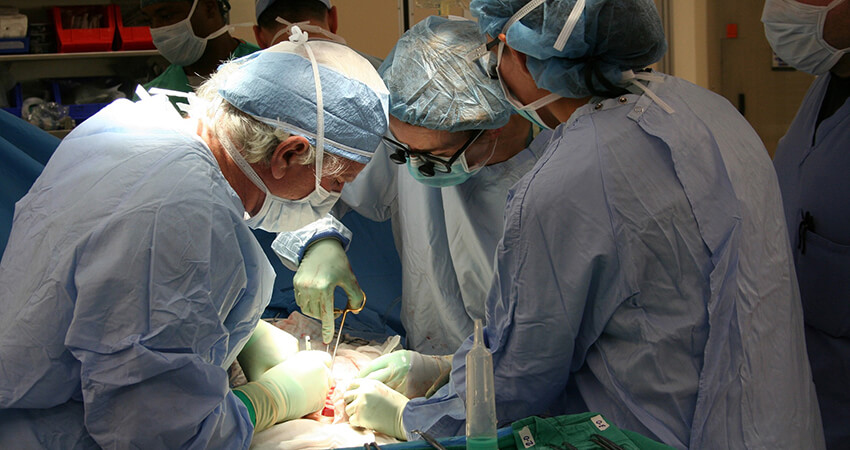
We collaborate in real-time across multiple disciplines to create a truly integrated and comprehensive path forward.
More Info

Utilizing the latest advancements in Machine Learning technology, we remove the "computer-wall" from between provider and patient.
More Info

We are resolved to advancing medicine by conducting superior phase 1 - 4 clinical research trials in pain management and neuroscience.
More Info
Excellence is the word.
We are the only real-time transdisciplinary support team in healthcare that truly delivers integrated medicine for the whole person, especially those with the most complex conditions, so that transformation happens.
Real-Time Transdisciplinary
We work together in the same room in order to blend disciplines, perspectives, and learning to create and shape personalized plans and solutions for each person.
The Whole Person
We are not just human bodies, we are human beings. In order to help someone achieve the best outcome, we must create a path to health that addresses the bio-psycho-social reality of each person.
Most Complex Conditions
Our approach will benefit everyone. This the way healthcare should be. However, we face an industry that doesn’t operate on the philosophy we adhere to, so our best chance at success is to focus.
Transformation
We create a personalized path for each patient and provide the direction, encouragement and tools they need to become a part of their own health care solution.
Book Appointment
Our real-time transdisciplinary team is dedicated to helping you find and follow your path to better health. Schedule your appointment today!
Pain Management Programs
Our offering of comprehensive healthcare programs features the full array of pain management services to diagnose and treat orthopedic, complex, and persistent pain conditions. Our goal is to reduce pain, improve function, and restore your quality of life.
Center of Excellence
The Center of Excellence is a Transdisciplinary Pain Program based on the Biopsychosocial model for the treatment of Chronic Pain.
Read More
Fee For Service
Our Fee For Service program offers traditional pain management services as well as several non-surgical interventional treatment options.
More Info
Surgery Centers
Our state-of-the-art surgical centers are outpatient facilities focused on providing high-quality care and advanced interventional techniques.
More Info Coming Soon
Treatments & Procedures
Many of our treatments show instant results. Call today for a consultation!
- MEDICATIONS: Opioids, NSAIDs, Muscle Relaxants, Anti-Convulsants, etc.
- INJECTIONS: Joint, Epidural Steroid, Nerve Blocks, etc.
- ADVANCED TECHNIQUES: Radiofrequency Ablation, Intrathecal Pump, Spinal Cord Stimulator
Want to prepare for your appointment early? Fill out your forms today!
Personal Stories
To us, you are more than a patient. You are a person. We work, not with patients, but with people to understand their roles in transforming their health. We create a personalized path for them and provide the direction, encouragement and tools they need to become a part of their own health care solution.
Here are some of their captivating stories!
Center of Excellence
Patient Testimonies
Try not to cry when you watch and listen to these powerful testimonies. These are people whose lives were in tough spot and were turned around through the treatments at Savas Health.
No More Pain Pills:
Viana's Story
Viana was in a bad car accident that caused her immense physical pain. Now after 9 months, she has not had to take a single pharmaceutical pill, using the all-natural methods from Savas Health.
Recovering Hope:
Marrion's Story
Marrion has a really special testimony to share about her experience at Savas Health. If you have 5 minutes to watch, please do. You will be very encouraged by her story.